QUESTION IMAGE
Question
question 7
1 pts
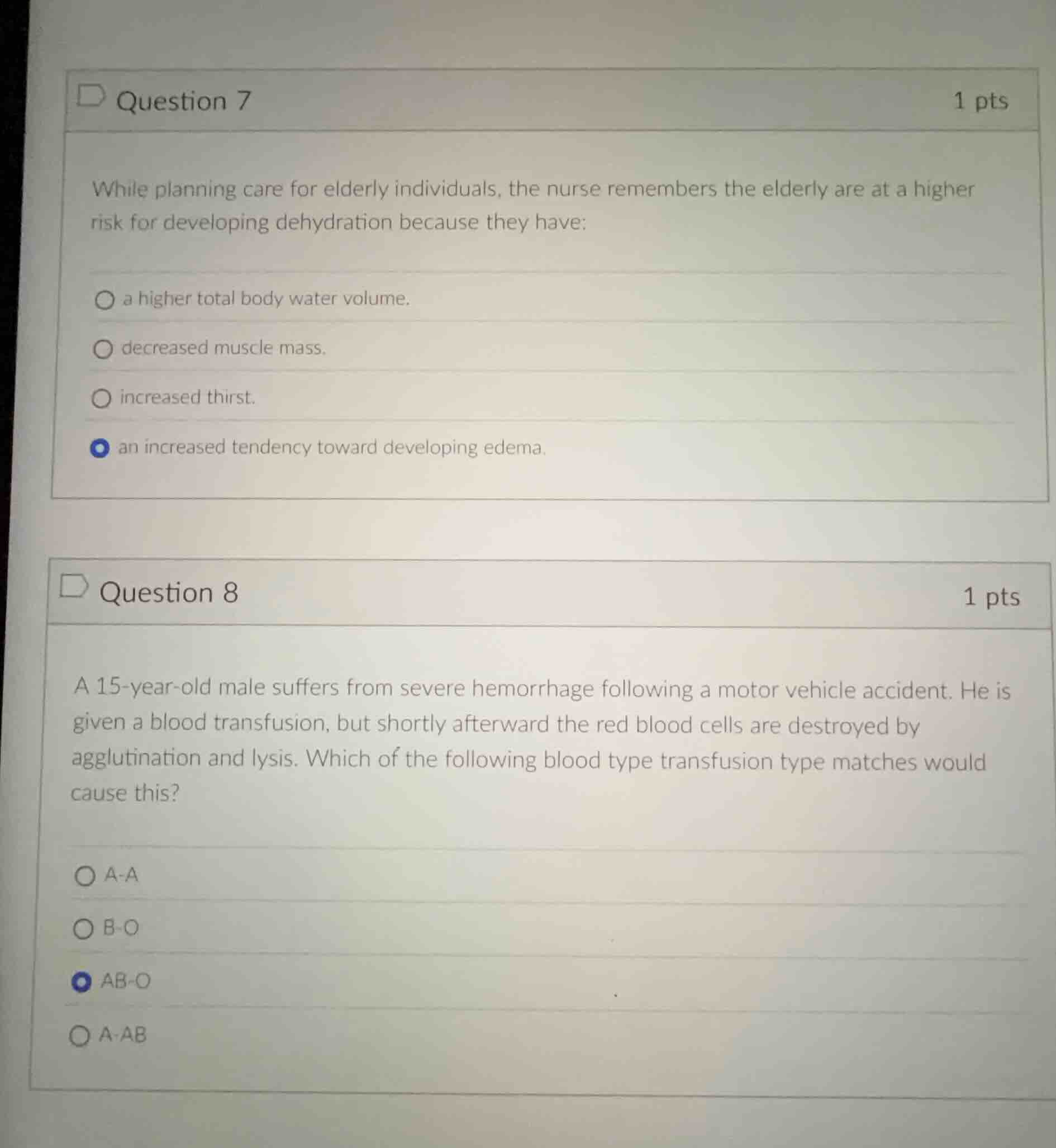
while planning care for elderly individuals, the nurse remembers the elderly are at a higher risk for developing dehydration because they have:
- a higher total body water volume.
- decreased muscle mass.
- increased thirst.
- an increased tendency toward developing edema.
question 8
1 pts
a 15-year-old male suffers from severe hemorrhage following a motor vehicle accident. he is given a blood transfusion, but shortly afterward the red blood cells are destroyed by agglutination and lysis. which of the following blood type transfusion type matches would cause this?
- a-a
- b-o
- ab-o
- a-ab
Question 7
To determine why the elderly are at higher risk for dehydration, we analyze each option:
- "A higher total body water volume" is incorrect because the elderly have a lower total body water volume (due to increased fat and decreased muscle mass, which has higher water content).
- "Decreased muscle mass" is correct. Muscle has a high water content, so less muscle means less water reserve. Also, the elderly have more fat (which has low water content), reducing overall water stores and increasing dehydration risk.
- "Increased thirst" is incorrect; the elderly often have a decreased thirst mechanism, making them less likely to drink enough.
- "An increased tendency toward developing edema" is incorrect. Edema (fluid retention) is not a direct cause of dehydration risk. Dehydration is about insufficient water, while edema involves abnormal fluid accumulation (often related to other issues like heart or kidney problems, not a primary dehydration risk factor for the elderly).
Blood transfusion reactions (agglutination/lysis) occur when the recipient’s antibodies attack the donor’s red blood cells (RBCs). We analyze each option:
- A-A: Recipient (A) has anti-B antibodies; donor (A) has A antigens. No reaction (donor RBCs have A antigens, recipient’s anti-B doesn’t target A).
- B-O: Recipient (B) has anti-A antibodies; donor (O) has no A/B antigens. No reaction (donor RBCs are “neutral”).
- AB-O: Recipient (AB) has no anti-A or anti-B antibodies (AB is the universal recipient). Donor (O) has no A/B antigens. Wait, no—wait, the question says the recipient is 15-year-old male (let’s assume the transfusion is donor to recipient). Wait, no: the recipient’s antibodies attack the donor’s RBCs. Wait, no—correction: If the recipient is AB and donor is O: AB recipients have no anti-A/anti-B, so they can receive any blood (O is universal donor). But the question says the RBCs are destroyed. Wait, maybe I mixed up donor and recipient. Wait, the problem says: “He is given a blood transfusion, but shortly afterward the red blood cells are destroyed by agglutination and lysis.” So the donor’s RBCs are being destroyed by the recipient’s plasma antibodies. Wait, no—actually, the recipient’s immune system (antibodies in plasma) attacks the donor’s RBCs. So:
- Recipient blood type determines the antibodies in their plasma.
- Donor blood type determines the antigens on their RBCs.
Let’s re-express each option (Recipient - Donor):
- A-A: Recipient (A) has anti-B in plasma. Donor (A) has A antigens. No reaction (anti-B doesn’t target A).
- B-O: Recipient (B) has anti-A in plasma. Donor (O) has no A/B antigens. No reaction (donor RBCs have no A to trigger anti-A).
- AB-O: Recipient (AB) has no anti-A or anti-B (AB plasma has no antibodies against A/B). Donor (O) has no A/B antigens. No reaction (AB can receive from O). Wait, this contradicts. Wait, maybe the option is reversed? Wait, the original option is “AB-O”—maybe it’s Donor AB, Recipient O? Wait, no, the problem says: “Which of the following blood type transfusion type matches would cause this?” So “X-Y” likely means Recipient X, Donor Y. Wait, no—common notation is Donor - Recipient? No, usually Recipient - Donor. Wait, no, standard is Donor blood type → Recipient blood type. Wait, let’s clarify:
- Universal Donor: O (no A/B antigens on RBCs, so recipient’s antibodies (if any) don’t target O RBCs).
- Universal Recipient: AB (no anti-A/anti-B in plasma, so doesn’t attack donor RBCs with A/B antigens).
Wait, the error in the initial thought: If the recipient is O, they have anti-A and anti-B. If donor is AB, donor RBCs have A and B antigens. Then O’s anti-A/anti-B would attack AB RBCs. But the option is AB-O (Recipient AB, Donor O)? No, that can’t be. Wait, the original option is “AB-O”—maybe it’s Donor AB, Recipient O? Let’s check the options again:
Options:
- A-A
- B-O
- AB-O
- A-AB
Ah! Wait, maybe the notation is Donor - Recipient (Donor blood type given to Recipient blood type). Let’s re-express:
- Donor A → Recipient A: Donor A (A antigens) to Recipient A (has anti-B). No reaction (anti-B doesn’t target A).
- Donor B → Recipient O: Donor B (B antigens) to Recipient O (has anti-A and anti-B). Anti-B in O’s plasma would attack B antigens. Wait, but option is B-O (Donor B, Recipient O)? But the option is B-O. Wait, no—let’s check the correct reaction:
The only way agglutination occurs is if the donor’s RBCs have antigens that the recipient’s plasma antibodies target.
- **Donor AB → Recip…
Snap & solve any problem in the app
Get step-by-step solutions on Sovi AI
Photo-based solutions with guided steps
Explore more problems and detailed explanations
B. decreased muscle mass